
Neurons - The Computer Chips Of Our Brain
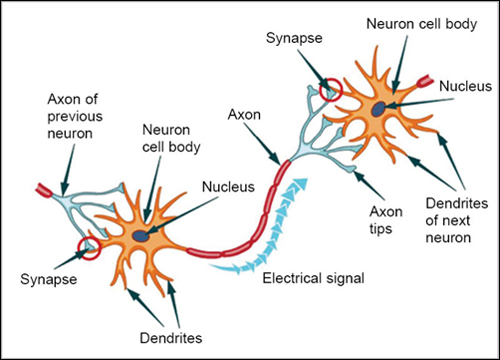
The brain is the most complex computer nature has evolved and the neuron is the chip that makes that computer go. Like a computer, the brain also has electrical connections. These impulses have been programmed by life to interpret and control all that human beings do.
Neurons are a far more brilliant component than today's computers. They communicate not in ones and zeros, but more likely in a code as complicated as our alphabet. In a single brain region, neurons may have billions of connections with other neurons.
Neurons are cells of the brain that are responsible for information transfer, both within the neuron itself and between other neurons. A neuron has these components:
- Soma, the cell body of the nucleus.
- Axons, the long electrical "transmission out" tube that in a neuron looks like a string of sausage casings and has at its end the transmission bulb.
- Dendrites, the complex antennas "receive" multiple signals transmitted from neighboring neurons.
Axons - The Communication Links Of Neurons
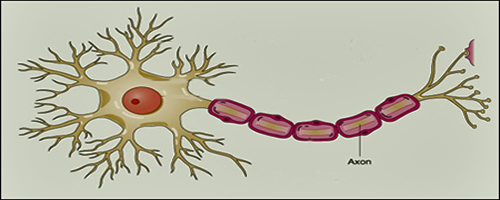
Axons are the long protrusions from the cell body of a neuron that transmit out the signals of a neuron to other cells in the body. The axon is essentially the neuron’s electrical wire. The axon channels allow electronically charged chemicals to reach the terminal end, which then creates an electrical charge moving the electrical signal down to the "axonal bulb" at the end of the cell.
There is only one axon per cell, but the end is very complex and can make contact with other cells, usually other neurons, but sometimes muscle or gland cells. Axons are microscopically small, but they run throughout the brain and the nervous system in groups, called axonal tracts, which can be seen by the naked eye. Some axonal tracts can extend up to one meter or more while others extend as little as one millimeter. The longest axons in the human body are those of the sciatic nerve which runs from the base of the spinal cord to the big toe of each foot.
From the axon ends, the signal then crosses the "synapse" (the junction between two brain neurons) to reach the next cell. The positively charged ion will drain its charge as it moves to the synapse, where it will have its signal boosted again. Unlike electrical insulation, the axon coating is not a continuous coating, but contains individually separated small cells. Between each juncture of the axon, there is a small gap in the insulation called the Nodes of Ranvier. These gaps serve an important purpose allowing energy to enter the axon to boost the electrical signal as it traverses the length of the link. Top
Glia Cells Are Critical For Neurons To Function
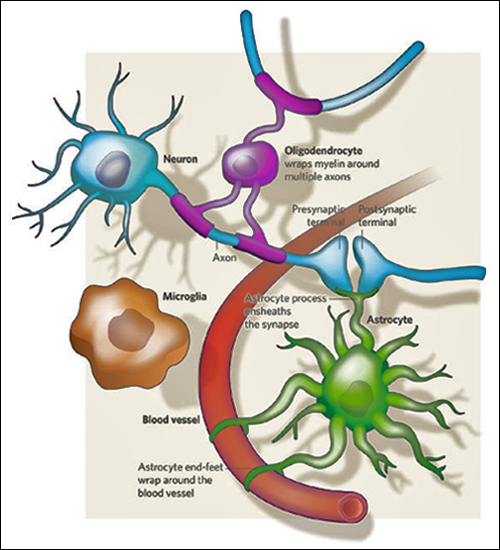
The defining characteristic of a neuron is its ability to transmit rapid electrical signals. All other neural cells that lack this property are categorized into a broad class called "glia".
Glia do not transmit action signals but instead surround and cover neuron cell bodies, axons and synapses throughout the nervous system. The human brain contains about nine glia cells for every neuron cell, i.e. our brains are 90% glia cells. Glia are essential to our brains, without them neurons die. There are three types of glia: oligodendrocytes, microglia, and astrocytes. Check out the purple, brown and green illustrations in the figure to the left.
The traditional view has been that glia look after neurons and maintain their proper functioning, having a somewhat passive role themselves. Established functions of glia include supporting neuro-transmission and insulating axons to speed up electrical communication. But resent research by Ben Barres and associates at Stanford University suggests that glia, particularly astrocytes, also have an "active role" in brain function and information processing.
Oligodendrocytes are the coatings on the cells that are spread end to end over the length of an axon. These glia cells resemble rolls of toilet paper, with the glia material wrapped many times around the core tube of the axon. Oligodendrocytes produce a non-soluble membrane called myelin, which wraps around axons and speeds up the conduction of electrical impulses.
Microglia, cells that fight diseases of the nervous system, survey the brain for any damaged and/or infected cells. They flow over and enclose all dead cells and debris. Microglia are also believed to be active during the development of the early nervous system removing inappropriate synaptic connections.
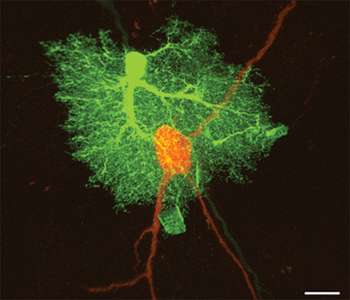
Astrocytes allow neurons to function. They contribute to a stable state of equilibrium in the brain by providing neurons with energy and substrates for neuron transmission. See the actual photo of an astrocyte cell (green) completely engulfing a neuron cell (orange) to the left.
Astrocytes act as physical barriers between the synaptic connections of neighboring neurons and remove excess neuro-transmitter molecules from the cellular space. This allows discrete and precise encoding of synaptic signals and neuro-transmission.
Recently, unexpected roles for astrocytes have been identified. They seem to be involved in the formation of synapses and in modulating synaptic functions through "bidirectional" communication with neurons.
Astrocytes control blood flow through their numerous processes which form close associations with blood vessels and neurons. In response to enhanced neuronal activity, astrocytes signal blood vessels the need for an increase in blood flow which then increases delivery of oxygen and glucose to an active brain region.
Besides regulating blood flow, astrocytes ferry glucose and oxygen from blood to neurons. It is hypothesized that they convert glucose into lactate. Lactate is then exported to neurons, where it is converted to pyruvate to produce the cell’s energy molecule ATP. Astrocytes communicate with each other through waves of calcium ions, propagating information over large distances. Stimulation of one astrocyte can cause a calcium response in a subset of neighboring astrocytes, with no response in other subsets. Bidirectional communication also occurs between neurons and astrocytes. Individual astrocytes can make contact with and cover up thousands of synapses formed between different neurons. Top
Our Brain Resets During Sleep
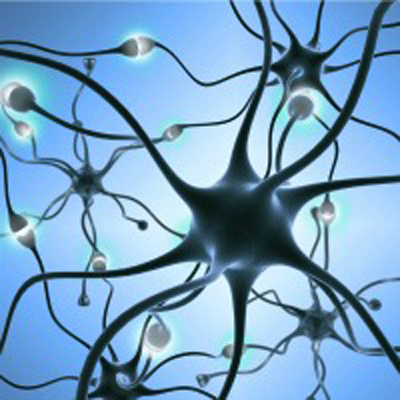
Researchers at the University of Wisconsin School of Medicine have tested a theory called Synaptic Homeostasis Hypothesis (SHY) for why humans need sleep. The four year study was published in the February, 2017 issue of Science magazine. SHY theory describes changes in synapses during waking and sleeping hours. See the illustration to the left. The large globs are neurons and the synapses are the junction connections (glowing white) between neurons. Our synapses grow strong and large during the stimulation of daytime, then shrink by nearly 20 percent while we sleep, creating room for more growth and learning the next day.
The larger the synapse, the stronger two neurons communicate. This ease of communication is how humans learn skills and retain memories. In order for brains to be pliable and learn new things, the synapses must shrink so the neural pathways can be activated again. According to SHY theory, sleep provides the environment for the shrinking of synapses allowing the brain to learn new things the following day.
The lack of stimulation while sleeping results in reduced activity between neurons. The size of the synapse grows smaller allowing them to be activated with a weaker stimulation. This phenomenon allows brains to make new neural connections the following day, thereby allowing new memories to form.
Researchers tested the SHY theory by measuring the size of synapses in a mouse study both before and after sleep. They utilized a three-dimensional scanning electron microscope to reconstruct the mouse brain and measured about 7,000 synapses. They specifically looked at neurons involved in motor functions and sensory perception. The team then repeated this process after the mice had slept and measured the synapses again.
The researchers found that the synaptic size correlated with the amount of sleep the mice had. The longer the mice slept, the smaller the synapses had become – with a few hours sleep resulting in a reduction of about 18 percent. Interestingly, the researchers only observed this phenomenon in about 80 percent of the synapses and that the largest of synapses appeared not to be susceptible to shrinking. They hypothesize that these large synapses might not follow the pattern because these synapses are associated with stable, long term memories and/or skills.
The results support SHY’s central tenant that the function of sleep is to re-normalize synapse size that increases throughout the day. The researchers theorize that the shrinking of the synapses might be related to the lack of neuro transmissions during sleep. The takeaway: Getting seven hours of sleep every night keeps human brains healthy. Top
Brain Plasticity
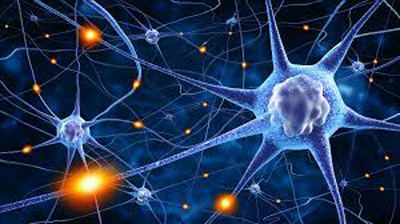
As you know, our brains are not made of plastic. Neuro-plasticity, or brain plasticity, refers to the brain’s ability to CHANGE throughout life. The human brain has the amazing ability to reorganize itself by forming new connections between brain cells (neurons). In addition to genetic factors, the environment in which a person lives, as well as the actions of the person, play a significant role in plasticity.
Below are some of the times when neuro-plasticity occurs in the brain:
- At the beginning of life: when the immature brain organizes itself.
- In the case of brain injury: to compensate for lost functions or to maximize remaining functions.
- Through adulthood: whenever something new is learned and memorized.
For a long time, it was believed that as we aged, the connections in the brain became fixed, and then simply faded. Research has shown that in fact the brain never stops changing through learning. Changes associated with learning occur mostly at the connections between neurons. New connections form and the internal structure of the existing synapses change. When you become an expert in a specific domain, the areas in your brain that deal with that type of skill grow.
An example: German medical students were imaged three months before their medical exam and right after the exam. They compared these to the brains of students who were not studying for an exam at that time. The Medical students’ brains showed learning induced changes in regions of the parietal cortex as well as in the posterior hippocampus. These regions of the brains are known to be involved in memory retrieval and learning.
A surprising consequence of neuro-plasticity is the fact that brain activity associated with a given function can actually move to a different location as a consequence of experience or brain damage. The brain compensates for damage by re-organizing and forming new connections between intact neurons. In order to reconnect, the neurons need to be stimulated by an activity. Top
The Gut-Brain Axis
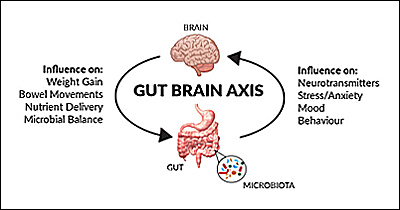
There is a growing body of work showing that there is communication between the gut and the brain, commonly called the gut–brain axis. The gut-brain axis is a bidirectional link between the central nervous system and the intestinal nervous system of the body. It involves direct and indirect pathways between thinking and emotional centers of the brain and non-digestive intestinal functions. See the illustrations to the left.
Microbiota is the name for the microbe population in a specific ecosystem, such as those found in the gut (or in the skin system, another example). Within the gut, there are approximately 10^14 micro-organisms, which is about 10 fold more than there are cells in the human body. There is mounting interest in determining how the gut microbiota can influence brain "disorders".
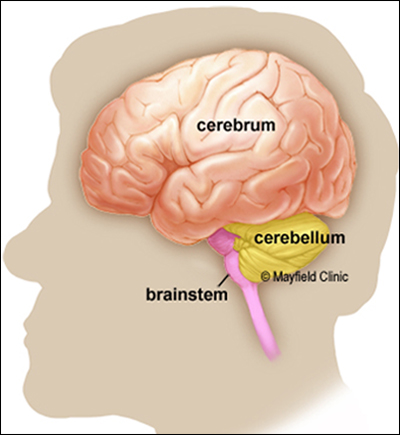
The Vagus nerve is the major mid-body transmitter to the brain and one of the longest nerves in the body. It is the main transfer agent that carries feedback from the intestine to the brainstem which in turn engages the hypothalamus and the limbic system (responsible for emotions). Similarly, descending Vagus impulses from the limbic system (activated by stress) influence gut activity.
The disruption of the gut–brain axis contributes to a diverse range of diseases, including Parkinson’s and irritable bowel syndrome. Consequently, the developing field of gut–brain axis research is rapidly growing and evolving.
New research shows an additional connection: immune signals sent from the gut can compromise the brain’s blood vessels, leading to deteriorated brain health and impairment of intellectual activity, such as thinking or remembering.
Surprisingly, the research unveils a previously unknown gut–brain connection mediated by the immune system and indicates that "excessive salt" might negatively impact brain health in humans by impairing the brain’s blood vessels.
Nearly every adult consumes too much salt! On average we take in 9 to 12 grams per day, about twice the recommended maximum intake of 5 grams by the World Health Organization.
The researchers experimented on mice and found that the immune responses in their small intestine set off a cascade of chemical responses reaching the brain’s blood vessels. This reduced the blood flow to the cortex and hippocampus, two brain regions crucial for learning and memory. In time, it brought a decline in tests for their brain performance.
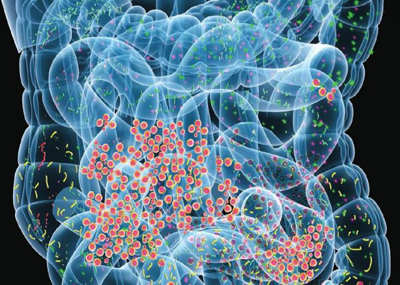
The researchers observed that the gut was reacting to a salt overload and then directed immune signals that were the basis for deterioration throughout the brain’s vascular complex which compromised thinking functions. While this study has only been carried out on mice so far, scientists believe it's likely that the results will apply to humans as well.
The good news is that when the mice were returned to a normal diet after being on a high salt diet, the detrimental health effects caused by excess salt intake were erased. An intervention that disrupted the immune signals also reversed the salt effects.
The implications of this gut–brain connection extend to several auto-immune disorders, including multiple sclerosis, psoriasis, rheumatoid arthritis and inflammatory bowel disease. These auto-immune disorders have a high stroke risk and are linked to poorly functioning blood vessels in the nervous system. This research demonstrates that what we eat can affect how we think. Top
DHA Keeps Our Brain Healthy
DHA (docosahexaenoic acid) is an omega-3 fatty acid found in fish oils that plays a central role in brain health. DHA is naturally found throughout the body, but is most abundant in the brain. Our brain is mostly fat, of which 60% is DHA. Just as calcium is essential for building strong bones, DHA ensures that the cells in the brain and other parts of the nervous system develop and function properly through all stages of life.
DHA not only turns on the growth of new brain cells, but offers protection for existing brain cells while it enhances the ability of one brain cell to connect to the next. DHA also acts as an anti-inflammatory. This is quite significant when one recognizes that inflammation is a key factor in both Alzheimer’s as well as Parkinson’s disease. And, DHA is active in controlling virtually every other neuro-degenerative condition.
A research team from the New Orleans School of Medicine in an April 2017 paper explained how DHA helps a damaged brain recover and keeps it functioning. Neuroprotectin D1 (NPD1) is a lipid messenger made from DHA on demand when cell survival is compromised. Oxidative stress, resulting from the constant production of damaging free radicals, lays the groundwork for cell death. Cell death is accelerated by catastrophic events like ischemic stroke.
The team found that about one hour after an experimental stroke, DHA triggered the production of NPD1. NPD1, in turn, increased the production of ring finger protein 146, which has been named Iduna. Iduna protects against a form of programmed cell death from stroke. Iduna, relatively little studied, turns out to be a key factor for cell re-programing and subsistence.
DHA is available as a supplement derived from fish oils as well as from marine algae. There is DHA in krill oil but the amount of DHA in krill oil is only about 10% of that found in fish oil. Eating fatty wild fish is a good source of DHA and clearly explains why fish is considered a “brain food.” DHA can be found in stores as a non-prescription supplement and can be purchased from Life Extension here. Top
Deep Brain Stimulation (DBS)
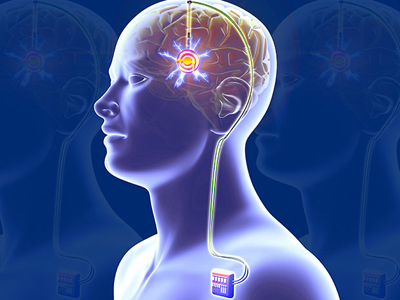
Deep Brain Stimulation, DBS, involves surgery for the implantation of electrodes deep inside the brain and then an electrical pulse generator sends stimulation pulses to the target area via microwires (the idea is similar to a heart pacemaker). This procedure was first introduced in 1987 on an experimental basis and was approved by the FDA in 1997 for treating Parkinson's Disease. About 150,000 Parkinson’s patients around the world have received an implant.
To treat Parkinson’s, the electrodes are placed in a brain region involved with movement. While the detail mechanisms of a DBS implant are still not clear, many researchers think the steady stimulating pulses override faulty patterns of normal electrical activity in certain regions of the brain.
DBS is currently being implemented on a very small sample of patients with "severe depression" on an experimental basis. For depression much research has centered on finding the proper targets for stimulation. The problem is that experimental trials have consistently had a subset of people who simply don’t respond to the treatment. So at this time, it has not been formally approved for severe depression any place in the world.
Recently at research center Emory University in Atlanta, 11 patients with severe depression who hadn’t responded to drugs, talk therapy, or electro-convulsive therapy, were given the DBS treatment. When all the patients were evaluated six months later, 8 of the 11 were judged to be responding well to the treatment. For one of the non-respondents, the researchers adjusted the parameters to better match the desired area of fiber activation. He got better quickly. Those that have had positive results stay better for very long periods of time - so far up to 10 years. For the two who did not respond, rearchers say depression is a complicated syndrome. There are probably some factors beyond the brain that need to be addressed.
In Germany, there is a 50-patient severe depression study expected to begin DBS implantations in the second half of 2017. If the results of this three-year trial are good, researchers believe that DBS treatment for depression will be on the path to regulatory approval in Europe. In the United States, regulatory approval requires a much more rigorous trial. Stay tuned. Top
10 Ways to Love Your Brain
Growing evidence indicates that people can reduce their risk of cognitive decline by adopting key lifestyle habits. When possible combine these habits to achieve maximum benefit for the brain and the body. Start now. It’s never too late to incorporate healthy habits. Here are 10 Ways To Love Your Brain as recommended by the Alzheimer's Association.
 |
Break a sweat. Engage in regular cardiovascular exercise that elevates your heart rate and increases blood flow to the brain and body. Several studies have found an association between physical activity and reduced risk of cognitive decline. |
 |
Hit the books. Formal education in any stage of life will help reduce your risk of cognitive decline and dementia. For example, take a class at a local college, community center or online. |
 |
Butt out. Evidence shows that smoking increases risk of cognitive decline. Quitting smoking can reduce that risk to levels comparable to those who have not smoked. |
 |
Follow your heart. Evidence shows that risk factors for cardiovascular disease and stroke — obesity, high blood pressure and diabetes — negatively impact your cognitive health. Take care of your heart, and your brain just might follow. |
 |
Heads up! Brain injury can raise your risk of cognitive decline and dementia. Wear a seat belt, use a helmet when playing contact sports or riding a bike, and take steps to prevent falls. |
 |
Fuel up right. Eat a healthy and balanced diet that is lower in fat and higher in vegetables and fruit to help reduce the risk of cognitive decline. Although research on diet and brain function is limited, some diets like the Mediterranean and DASH diets, contribute to risk reduction. |
 |
Catch some Zzz's. Not getting enough sleep due to conditions like insomnia or sleep apnea may result in problems with memory and thinking. |
 |
Take care of your mental health. Some studies link a history of depression with increased risk of cognitive decline, so seek medical treatment if you have symptoms of depression, anxiety or other mental health concerns. Also, try to manage stress. |
 |
Buddy up. Staying socially engaged may support brain health. Pursue social activities that are meaningful to you. Find ways to be part of your local community — if you love animals, consider volunteering at a local shelter. If you enjoy singing, join a local choir or help at an afterschool program. Or, just share activities with friends and family. |
 |
Stump yourself. Challenge and activate your mind. Build a piece of furniture. Complete a jigsaw puzzle. Do something artistic. Play games, such as bridge, that make you think strategically. Challenging your mind may have short and long-term benefits for your brain. |